Vein Disease Treatment in Ithaca, New York
Varicose Veins
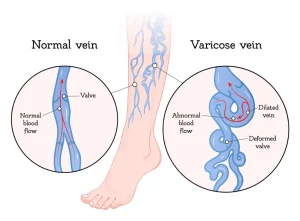
Varicose veins are large, swollen veins that often appear on the legs and feet and may be a sign of venous reflux disease. Healthy leg veins have valves that keep blood flowing toward the heart. When varicose veins appear, it can be a result of valves not working properly. This can cause the blood to flow backward and pool in the lower legs.
The signs and symptoms of venous reflux disease include:
- Varicose veins
- Aching
- Swelling
- Cramping
- Heaviness or tiredness
- Itching
- Restlessness
- Open Skin Sores
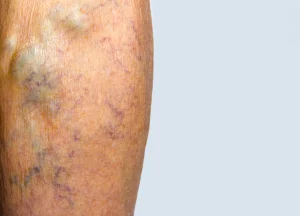
Varicose veins are not just a cosmetic problem. If left untreated, over time varicose veins can worsen and lead to other issues including phlebitis, blood clots, skin changes, and leg ulcers.
Risk factors associated with varicose veins include:
- Prolonged sitting or standing
- Pregnancy
- Family history
- Female gender
- Obesity
- Tall height
Spider Veins
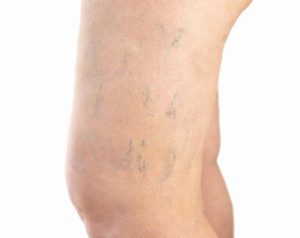
Spider veins are small veins that appear just under the surface of the skin. They can be blue, red, or purple. They can be associated with varicose veins and can be the result of faulty valves. Women are more susceptible to spider veins related to hormone levels. Changes in hormone levels can reduce how well the valves work and can also weaken the vein walls. Blood then builds up in the vein causing them to bulge just below the surface of the skin.
Stasis Dermatitis and Leg Ulcers
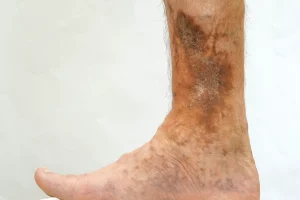
When valves malfunction, blood flows backward and pools in the lower legs. This causes increased pressure and swelling in the veins.
As the fluid and pressure build, some of the blood leaks out of the veins and into the tissues. This leads to venous stasis skin changes, sometimes referred to as stasis dermatitis. Symptoms associated with stasis dermatitis include skin discoloration, itching, and scaling.
When stasis dermatitis becomes advanced, it can lead to a venous leg ulcer. Venous leg ulcers are sores on the leg that take a long time to heal. They occur between the foot and the calf, typically around the ankle. Symptoms include swelling, itching, worsening pain, and drainage coming from the sore. Treatment usually consists of compression therapy and the ulcer can take months to heal. If your ulcer is the result of venous disease, treating the underlying cause can prevent recurrence.
Superficial Thrombophlebitis
Phlebitis is the inflammation of a vein. If the inflammation is related to a blood clot it is called thrombophlebitis. Superficial thrombophlebitis is a clot in the superficial venous system. Symptoms of superficial thrombophlebitis include pain, swelling of the extremity, feeling of warmth, and red or discolored skin in the area of the clot. Common causes include prolonged activity such as long drives or plane rides, varicose veins, local trauma to the vein, and an underlying clotting disorder. Diagnosis is made by physical examination and ultrasound. Treatment generally consists of applying warm compresses, elevating the affected extremity, walking, and oral anti-inflammatory medications. If venous reflux is suspected as the cause, treatment is available to prevent future episodes.
Deep Venous Thrombosis
When a blood clot occurs in a deep vein it is called a deep vein thrombosis (DVT). This is more serious than superficial thrombophlebitis because these clots can break off, travel to the lungs, and become life threatening. The symptoms of DVT include swelling, pain, warmth, and redness. The causes can be related to inactivity, trauma, certain medications, or a blood clotting disorder. If deep venous thrombosis is suspected, you should immediately be evaluated by your physician. Drugs called anticoagulants (blood thinners) are the most common treatment for a DVT.
Schedule A Consultation Today!
Interested in learning more about our available vein treatments? Call 866-257-1818 to schedule your consultation with Dr. Ferrer today! Our practices serves Ithaca, Horseheads, & more in New York
